 Update: I am not the first to write about this area. I found a great post by Todd Hargrove tackling the same topic and saying much the same (he does it more succintly and I address a few other areas as well). His post is here: http://www.bettermovement.org/2011/does-excessive-sitting-shorten-the-hip-flexors/
Update: I am not the first to write about this area. I found a great post by Todd Hargrove tackling the same topic and saying much the same (he does it more succintly and I address a few other areas as well). His post is here: http://www.bettermovement.org/2011/does-excessive-sitting-shorten-the-hip-flexors/
The Tight Hip Flexor Bogeyman
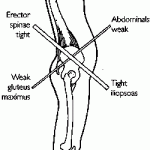
We too often tell patients that their pain, dysfunction or poor performance on any movement is due to the great bogeyman of hip function - TIGHT HIP FLEXORS. It is quite a go-to explanation for all things bad. Where this idea started I don’t know but it is certainly propagated by the Lower Crossed Syndrome Theory. This theory contends that dysfunction occurs when your pelvis is tilted forward as a result of tight hip flexors, weak glutes, tight low back muscles and weak abs. At its heart, this theory assumes the body works like a puppet where we can tension and loosen our strings (aka muscles) and watch our pelvis dance into some assumed nasty or happy position.
What is the theory behind tight hip flexors
 A common explanation (and from people I respect very much) for the assumed tight hip flexors is our 20th century sedentary lifestyle. This explanation contends that if we sit for eight hours a day at our desks our hips will be flexed, the hip flexors will be constantly short and we will then cause those hip flexors to stay short. While this is an attractive theory I just can’t buy it. I have a 15 year gripe with this theory and with the other unsupported functional beliefs that then arise from this theory. So here goes.
A common explanation (and from people I respect very much) for the assumed tight hip flexors is our 20th century sedentary lifestyle. This explanation contends that if we sit for eight hours a day at our desks our hips will be flexed, the hip flexors will be constantly short and we will then cause those hip flexors to stay short. While this is an attractive theory I just can’t buy it. I have a 15 year gripe with this theory and with the other unsupported functional beliefs that then arise from this theory. So here goes.
Can sitting all day tighten your hip flexors? I say no way. Here’s why.
1. Even if you did sit for a straight, uninterrupted 8 hours a day this isn’t enough to create shortening in muscle tissue. Shortening occurs when you are in a cast, immobilized in someway in a shortened position for prolonged periods. I mean days and weeks. 8 hours ain’t jack. Even with an hour day you aren’t really stuck in that position. You get up throughout the day and stand up, thus interrupting the shortening possibilities.
2. If this 8 hours is so horrible you would negate this when you sleep for 8 hours with your legs straight or during all of your other upright activities. On the opposite side of that wouldn’t we be more likely to shorten our hip flexors if we sleep in the fetal position for 8 hours a night? Is no one telling their patients to stop sleeping on their sides with their knees up? Speaking of Fetuses aren’t they scrunched up in ball for 9 months? Shouldn’t they have decreased hip extension?
3. The argument against our sedentary culture is often contrasted with other cultures that choose to sit differently than us. With these cultures we celebrate their deep squat. Should we be worried about them sitting in a deep squat for prolonged periods? Won’t their hip flexors shorten? I will send a telegram immediately with these warnings.
Possible contentious extensions of the Tight Hip Flexor Theory
If you support the tight hip flexor theory than logically there are many ways that this will shape how you view muscle function and movement.
1. An inappropriate use of reciprocal inhibition.
By my interpretation I think that this occurs with us therapists inappropriately applying Sherrington’s law of reciprocal innervation (aka reciprocal inhibition). It is often concluded that a tight hip flexor will cause an inhibition of one its antagonists, the Gluteus Maximus. However, we can argue against this use in two ways.
1. reciprocal innervation requires that a motor command to an agonist is associated with some inhbition of its antagonist. The proposed tight hip flexor secondary to prolonged sitting is not due to some tonic muscle contraction of the hip flexors but rather changes in the passive length of the hip flexor. There is no neural drive that creates the shortening therefore no means for the reciprocal innervation to occur.
2. Even if there is neural drive to an agonist it may not be sufficient to create any significant inhibition of its antagonist. This is not how reciprocal innervation works. A great review and full text paper can be seen here. Reciprocal inhibition typically occurs greatest at a reflexive level during gait rather than during volitional movements. I am not even sure if it has been documented when we try to test the strength of the “inhibited” muscle because once we do this that antagonist that was supposedly being inhibited is now the agonist. Further, muscular co-contraction is pretty much the norm during many activities. We contract (think hamstrings and quadriceps at the knee) to provide stability and controlled movement. If reciprocal inhibition worked in the manner suggested by the tight or overactive hip flexors than it would be difficult to obtain the stability required in joints via co-contraction. To conclude, I don’t think that any evidence that reciprocal innervation leads to weakness as is postulated exists. However, I am open to hearing some research that I don’t know about. I wonder if this paper here pokes holes in my ideas (my guess is no, I actually think it strengthens it) but I think that this paper here looking at neuromuscular adaptations to stretching definitely strengthens it.
2. Tight Hip Flexors need to be released
I have had my hip flexors “released” by several ART instructors and never thought they actually touched my psoas. At least the deep component of that muscle. They definitely squeezed my guts and beat the shit out of three layers of abdominal muscles and maybe some intestine or omentum but they didn’t “release” my psoas by poking it. And how could 3 minutes of a psoas release influence years of 8 hours a day of sitting posture via mechanical means? Neural mechanism? Absolutely but no one is touting this theory. We might also consider what attempting to stretch the psoas can actually result in if we consider the limits of stretching on changing long term muscle stiffness and therefore resting length. See a brief post here on stretching and muscle.
3. Believing in tight hip flexors can lead to the danger of hip (over)extension.
I am subject to confirmation bias. I have a view of the body that changes constantly but also informs what I see in my patients and what I do. if you believe in the lower cross syndrome than you go looking for it. You then want to increase extension because that is the natural follow up of diagnosing this clinical entity. But I would contend that stretching or treating into hip extension may be detrimental to your patients or athletes. Please see my post on the dangers of hip extension. It is akin to cranking a shoulder into abduction and external rotation…what are you doing to the anterior capsule? Is this an adaptation or a stress that you want to place on everyone?
4. Why do you want hip extension? How much do you need?
You need 10-15 degrees during walking and you need about the same amount during running. Hip extension is over rated. Related to this, you don’t even use your glut max during walking to extend your hip and during running you don’t use your Glut max to extend your hip past zero degrees. By the time your leg swings back, is on the ground and starts to extend past neutral the glutes have shut off. That’s the extensor paradox dude.
5. A caveat of possible clinical relevance: Hip Extension during running is related to anterior pelvic tilt.
There is a neat paper from JR Franz and one by Schache et al (2000) showing that limited hip extension during running is coupled with increased lumbar lordosis. The authors suggest that this is related to injury. I have three points on that:
1. Whether this is related to injury or performance decrement has not been tested and is purely conjecture.
2. Your tests for measuring hip extension (e.g. Thomas test) do not correlate with the amount of hip extension that occurs during running ( full text here Schache et al 2000). Meaning, while running you might not extend your hip and this will be related to an increased anterior pelvic BUT this is not due to you having tight hip flexors. Less hip extension availability was not correlated with anterior pelvic tilt. This is a great example of how the kinematics of quasi-static tests of function (e.g. Thomas test, one leg squat) don’t often correlate with the kinematics that occur with dynamic function during tasks of interest (e.g. running). Our motor planning may choose to limit your extension rather than a physical limitation tested during the Thomas Test. You are going to have eyeball your video of them running to see if your athlete lacks hip extension. Good luck doing that accurately.
3. The increased anterior tilt is not a function of a tight muscle pulling the pelvis into a new position. Rather the tilt may occur because the thigh must extend and it can do this in two ways. Hip extension or pelvic tilt. Some individuals seem to involuntarily choose to do this with more pelvic tilt and they therefore don’t need to extend their hip.
Final Thoughts
1. I think that tight hip flexors are overdiagnosed. The thomas test may even test something besides hip flexors and produce false positives (no reference et al 2012). I often test patients in prone and just pull their leg into extension. I rarely see a loss of movement.
2. I certainly don’t think that even eight hours of sitting can shorten your hip flexors.
3. The perception of hip flexor “tightness” may be just that, a perception. Tight does not have to mean short it can just be a way for your brain to tell that something feels off.
4. Tightness or lack of range may exist but does not have to be something so mechanical. We have a nervous system and range deficits may be related to guarding or threat behaviour.
5. All of the techniques used to address the lower cross syndrome can still be wonderful for treating your patient’s pain or dysfunction. We don’t need to throw the treatment baby out with the dirty psoas bathwater.
Adios,
Greg
Two neat papers that I don’t have but want on reciprocal inhibition and stretching.
1. Hayes et al Neuromuscular Origins of Adaptation do not Exist Following a Long-term Stretching Program. J Sport Rehabil. 2012 Mar 2. [Epub ahead of print]
2. Blazevich AJ, Kay AD, Waugh C, Fath F, Miller S, Cannavan D. Plantarflexor stretch training increases reciprocal inhibition measured during voluntary dorsiflexion.J Neurophysiol. 2012 Jan;107(1):250-6. Epub 2011 Oct 5.




[...] Are you sure your hip flexors are tight? If so, why and who cares … [...]
Thanks for this Greg.
Low back health aside, I find this comment interesting from a performance standpoint as it pertains to sprinting:
“The increased anterior tilt is not a function of a tight muscle pulling the pelvis into a new position. Rather the tilt may occur because the thigh must extend and it can do this in two ways. Hip extension or pelvic tilt. Some individuals seem to involuntarily choose to do this with more pelvic tilt and they therefore don’t need to extend their hip.”
Have a look at this gentleman’s anterior tilt http://www.youtube.com/watch?feature=player_embedded&v=TSsiUyMR-gw I’m sure he also doesn’t have a 90 degree SLR and I for one wouldn’t want to try an improve it for him.
Thanks Jeff,
Great insight. I’ve seen that video before, blows my mind. Its like his lumbar lordosis begins at T9.
Sprinters are good example of not needing full hip extension. There is some research showing that a faster runners and a transition to faster speeds is accompanied with less hip extension and greater and faster hip flexion. As if, the leg is trying to get off the ground sooner during hip extension and they don’t want it to lag back there (during extension).
Greg
[...] as a result of following the lower crossed syndrome hypothesis. So I was interested to read Greg Lehman’s post about hip flexors and whether they really can be made tight by a sedentary lifestyle. I liked the [...]
Hi Greg,
Thank you very much for the link. And great job on the article, you make some excellent points that I missed. By the way we are of like minds on the foam rolling issue as well. Perhaps I will do my own post (with a link to yours of course.)
Would love to hear your insights into rolling. I recognize that so many people promote it and many love it. I just wonder if this is still the best use of our time. I mean are you better off trading that ten minutes of foam rolling with ten minutes of wrestling yourself into compression tights or even boring old icing (at certain times in your training cycle).
All the best,
Greg