Audience: Health Professionals and Patients
Source of Information: Paula Ludewig, Ben Kibler, Ann Cools, Rafael Escamilla, Mike Reinold, Kevin Wilks
Disclaimer: The information below really just scratches the surface. References at the end of post are excellent. The point of this post is to get people to think more about culprits of dysfunction when it comes to the shoulder rather than just labeling shoulders with victim diagnoses (e.g. bursitis, tears, “tendinitis” - I hate that word - a future post will address my disdain).
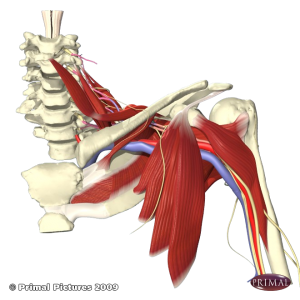 Shoulder Impingement is not a diagnosis. It is a finding and can be both a cause and the result of dysfunction. Impingement is pretty much what it sounds like - something is getting pinched. Ever reach into your back seat or reach to put your coat on and feel a sharp pain somewhere around your shoulder (and often down to your elbow). That is impingement. Some structure under the shoulder blade is getting pinched and does not like it. Who likes to get pinched?
Shoulder Impingement is not a diagnosis. It is a finding and can be both a cause and the result of dysfunction. Impingement is pretty much what it sounds like - something is getting pinched. Ever reach into your back seat or reach to put your coat on and feel a sharp pain somewhere around your shoulder (and often down to your elbow). That is impingement. Some structure under the shoulder blade is getting pinched and does not like it. Who likes to get pinched?
I crudely categorize shoulder impingement into two categories (although they can be split to a greater extent as well) - 1. Internal impingement and 2. External Impingement.
Internal Impingement - what is pinching?
- rotator cuff muscles (Supraspinatus and Infraspinatus) get pinched against the upper-back (and even the upper front) portion of the Glenoid/Labral complex during shoulder abduction and external rotation. This is essentially the position of throwing or reaching to put your coat on.
- less commonly, the subscapularis muscles (an internal rotator cuff muscle) can get pinched between the corocoid process and the lesser tuberosity of the humerus
External Impingement - what is pinching?
- pinching of the rotator cuff tendons or long head of the biceps brachii on any part of the coracoacromial arch (i.e. the underside of the front of the shoulder blade). This arch consists of the coracoacromial ligament, the acromial undersurface and the undersurface of the AC joint.
The aim of treatment - Stop the pinching stupid.
The end goal of treatment is simple. Get the surfaces that are pinching each other out of each other’s way. When my 3 year old pushes over my 10 month old I don’t leave them beside each other. With impingement treatment we are trying to make space - Space can be made in two ways:
1. Get the arm bone out of the way (some will call this joint centration) by optimizing rotator cuff function.
2. Get the shoulder blade out of the way. We will try to put the shoulder blade in an optimal position.
How do we make space?
I typically use a lot of manual therapy. An extensive amount of Active Release Technique, trigger point holds, acupuncture/dry needling, contract-relax, PIR, spine manipulation, A-P mobilizations etc. I tend to treat any structure that can influence the shoulder and less scientifically, “feels not normal”. Because that is a lot of the magic of manual therapy - we do a subjective evaluation of tissue texture, “vitality”, robustness, springiness, ropeyness, adhesions etc and work those areas. I will treat all “faulty” tissue that attaches to the shoulder, the neck and the back.
One caveat, I tend to avoid stretching the front of the shoulder. I kept seeing weight lifters (i.e. bench pressers) with internal impingement but they thought they were protected because of stretching the crap out of the front their shoulder and then busting out a deep bench press. Avoid this please. This may cause anterior laxity which then allows the the humeral head to translate into a pinching position.
But Manual Therapy is just the start:
In order to make long lasting change we need to change how the shoulder complex functions. It is through rehabilitation exercises (both supervised/corrected and at home) that we can essentially teach the shoulder and spine musculature to again work like the good team that they are and stop the pinching. Because it is often the loss of teamwork that is the problem. A shoulder might have an incredible amount of strength but certain positions or movements cause an equally incredible amount of pain. Lots of strength does not equal a healthy shoulder. What is mostly likely happening is that something is wrong with how the body moves and optimal body movement is a result of good teamwork by the muscles.
Below is a quick overview of some components of the rehabilitation regime. Part two of the post will delve a great deal into the science and research behind appropriate exercise prescription.
Overview of elements that might be incorporated (if needed)
1. Check and train spine stability - people should be doing lower spine exercises so why not introduce McGill’s big three or some other program for the spine that you like.
2. Stretch pectoralis minor (decreases anterior tilting of scapula to make more space underneath)
3. Check and treat deep neck flexor inhibition (perhaps the patient is using the superficial neck muscles excessively which then anteriorly rotates the scapula or inhibits movement of the clavicular - again this can decrease space. **Please note, I don’ t think there is any research (despite the almost universal acceptance of the upper crossed syndrome) on this but it is not unreasonable to think that alterations in how the neck moves can negatively affect how the shoulder blade moves.
4. Teach the external and internal rotator cuff muscles to “play catch” with one another. One theory on dysfunction is that the rotator cuff no longer works as a team and then no longer centres the arm bone under the shoulder blade. Working the arm in external and then internal ranges can facilitate these muscles. Follow this with…
5. External rotator cuff strengthening at neutral first and then all ranges of elevation.
6. Posterior capsule stretching (e.g. sleeper stretch, cross body adduction).
7. Serratus anterior strengthening
8. Scapular positioning exercises (learning how to move the scapula into different positions - up, down, back, forward)
9. Teach diaphragmatic breathing (Why not, everything is connected)
A future post will explore in much greater detail shoulder rehabilitation exercises. This next post will focus much on the work of Ann Cools, Mike Reinold (www.mikereinold.com), Paula Ludewig and Rafael Escamilla. I take no ownership of the research - I am just an early adopter and respect the science and thought behind their exercise prescriptions.
UPDATE: As goes with the internet there is a tonne of redundancy. Please see the following link from Mike Reinold who made a great post on impingement way back last year and way before me. Dr Reinold is also involved in the research attempting to understand shoulder pathology so it is nice and prudent to go to a primary source. http://www.mikereinold.com/2010/11/shoulder-impingement-3-keys-to.html
References
1. Ludewig PM, Braman JP. Shoulder impingement: biomechanical considerations in rehabilitation. Man Ther. 2011 Feb;16(1):33-9.\
2. Cools AM, Cambier D, Witvrouw EE.Screening the athlete’s shoulder for impingement symptoms: a clinical reasoning algorithm for early detection of shoulder pathology. Br J Sports Med. 2008 Aug;42(8):628-35. Epub 2008 Jun 3. Review
3. Reinold MM, Escamilla RF, Wilk KE. Current concepts in the scientific and clinical rationale behind exercises for glenohumeral and scapulothoracic musculature. J Orthop Sports Phys Ther. 2009 Feb;39(2):105-17. Review.
4. Kibler WB, Ludewig PM, McClure P, Uhl TL, Sciascia A.Scapular Summit 2009: introduction. July 16, 2009, Lexington, Kentucky. J Orthop Sports Phys Ther. 2009 Nov;39(11):A1-A13. Review.
5. Escamilla RF, Yamashiro K, Paulos L, Andrews JR.Shoulder muscle activity and function in common shoulder rehabilitation exercises. Sports Med. 2009;39(8):663-85. Review.




[...] a previous post (http://thebodymechanic.ca/2011/01/18/shoulder-impingement-rehabilitation-part-one/), I briefly touched on some components of shoulder rehabilitation. In this post I wanted to [...]